19 . 07 . 2019
Helicobacter pylori Infection and Autoimmune Thyroid Diseases - is there an association?
The thyroid is the most affected organ by autoimmune disease. Although thyroid autoimmunity’s etiology is multifactorial, there is evidence that some infectious agents, including Helicobacter pylori, may contribute to its development.
Helicobacter pylori (Hp) is a gram-negative bacteria with the ability to colonize and infect the gastric mucosa. This infection is quite common, being present in about half of the world’s population. The local consequences of Hp infection are gastritis, peptic ulcer, and gastric carcinoma. However, some extra digestive manifestations such as idiopathic thrombocytopenic purpura (a disease characterized by autoimmune destruction of platelets) and even atherosclerotic coronary disease have been associated with the presence of Hp, in the medical literature.
What are autoimmune thyroid diseases?
Autoimmune thyroid diseases (ATDs) are very common, with an estimated prevalence of 5% in the population (women are more affected than men). ATDs characterized by the presence of antibodies directed against the thyroid tissue, and lymphocytic infiltrates in the gland. This immune reaction leads to the progressive destruction of the gland, which can then cause functional changes (hypo or hyperthyroidism). The two main ATDs are the following:
- Hashimoto’s thyroiditis – antibodies against thyroglobulin (Anti-Tg) and thyroperoxidase (Anti-TPO) are generally present. Due to the gland’s progressive destruction, hypothyroidism usually ensues after a few years.
- Graves’ disease – the presence of TSH receptor-specific antibodies (TRAb’s) promotes hyperstimulation of the gland, which causes hyperthyroidism.
What causes these diseases?
As with other autoimmune diseases, the cause is not known. A combination of genetic and environmental factors can trigger autoimmunity. Exposure to certain drugs, iodine, smoking, and possibly stress, contributes to the development of ATD. Certain viral and bacterial infections, such as Hepatitis C, Coxsackie virus, Yersinia enterocolitica, Borrelia burgdorferi, and Helicobacter pylori, have also been proposed as possible autoimmune triggers.
How can an infection promote autoimmunity?
Infectious agents activate the immune system, which tries to control and eradicate them. This process is dynamic and more complicated than it may seem. Microorganisms can “confuse” our immune system, causing it to react against molecules and tissues of the body itself. Several mechanisms explain this phenomenon, such as molecular mimicry (similar molecules between the microorganism and the host), modification of host antigens due to interaction with the infectious agent, and excessive stimulation of immune cells.
Is there an association between Helicobacter pylori infection and ATDs?
Over the past 20 years, multiple studies have tried to answer this question with different results. A meta-analysis published in 2017 looked at 15 articles (a total of 3046 patients) and found a positive association between Hp infection and autoimmune thyroid disease (OR-2.25, which means that an infected person has a risk 2.25-fold higher risk of developing ATD). This association was more significant in Grave’s disease (OR-2.78) than in Hashimoto’s thyroiditis (OR-2.16).
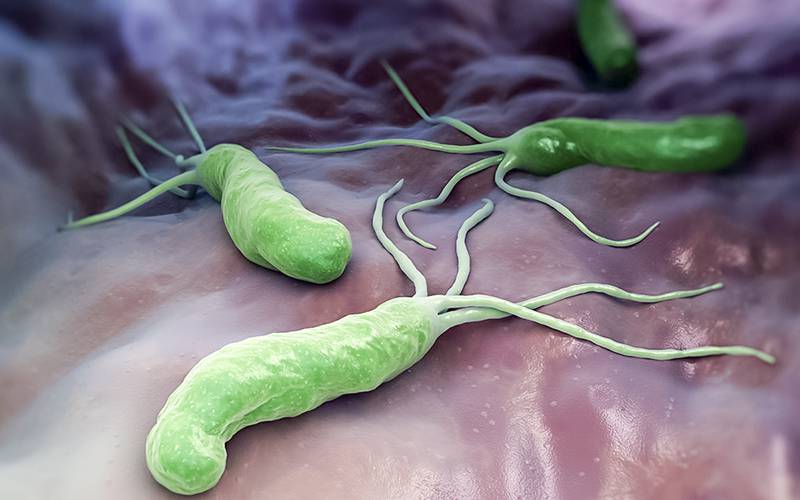
Fig. 1 – Helicobacter pylori is a Gram-negative bacteria that infects the mucosa of the stomach.
How does this likely association influence clinical practice?
In the case of autoimmune thyroid disease, the conventional treatment is to replace thyroid hormone levels when there is hypothyroidism (Hashimoto), or to suppress the endogenous production of the thyroid when there is hyperthyroidism (Graves’ disease).
However, in parallel, it is important to identify and correct potential factors that may contribute to autoimmunity. The association between Hp infection and ATDs is suggested in the literature, and there is, at least, one study reporting a significant decrease in anti-thyroid antibodies after Hp eradication. This was a small study with only 10 patients, but it raises an important question for the clinician: Is eradication of Hp indicated in patients with ATD’s?
Autoimmune diseases are complex, and it is important to have a comprehensive view of the different factors that may have triggered their manifestation. Certain infections, such as Helicobacter pylori, fall in this category.
References:
Hou Y, Sun W, Zhang C, et al. Meta-analysis of the correlation between Helicobacter pylori infection and autoimmune thyroid diseases. Oncotarget. 2017;8(70):115691–115700.
Köhling HL, Plummer SF, Marchesi JR, et al. The microbiota and autoimmunity:Their role in thyroid autoimmune diseases. Clinical Immunology. 2017;183:63-74.
Shmuely H, Shimon I, Gitter LA. Helicobacter pylori infection in women with Hashimoto thyroiditis: A case-control study. Medicine (Baltimore). 2016;95(29):e4074.
Bertalot G, Montresor G, Tampieri M, et al. Decrease in thyroid autoantibodies after eradication of Helicobacter pylori infection. Clinical Endocrinology (Oxf). 2004;61(5):650-652.
Thank you for this. I suffer from Graves, which came on after years of various gastric issues, chiefly GERD – and was only recently dx’d with h pylori. My sibling has the counter to Graves – Hashimoto – and was also dx’d with this bacteria… If only the medical establishment had thought of looking for h pylori as the cause of the gastric issues, maybe we would’ve faced a better outcome on the autoimmunity front. Currently I’m strongly considering thyroid removal after 5 years of anti-thyroid medication, and wish there would be more info available on the course of Graves ophthalmopathy post-thyroidectomy, so I can make a more informed decision.
Hi Gia.
There could be a relationship there but it’s impossible to know now.
The digestive system’s health is key to a balanced immune system.
You may still benefit from working with a functional medicine doc to see if there’s a way to ease the Graves.